Just ask football legend John Elway, who struggled with gastroesophageal reflux disease (GERD) for more than a decade. “I was totally in the dark about acid reflux,” Elway told the Post. “No one should tough it out like I tried to do.”
Not only does the uncomfortable condition land many people in the hospital, but over time the repeated exposure to stomach acids can irritate and inflame the lining of the esophagus, increasing one’s risk for ulcers and esophageal cancer, a rare but deadly complication of GERD.
That’s the bad news.
There’s good news, too. Gastroenterologists say public awareness of GERD is on the rise. More people are seeking medical help and screenings for complications.
“Today, the public is clearly more aware of the potential importance of heartburn as a symptom of disease and not a trivial item” blamed on overeating, says Dr. Philip Katz of Albert Einstein Medical Center in Philadelphia. And more of us understand that a small percentage of people with chronic reflux symptoms are at risk of serious complications, including cancer, he says.
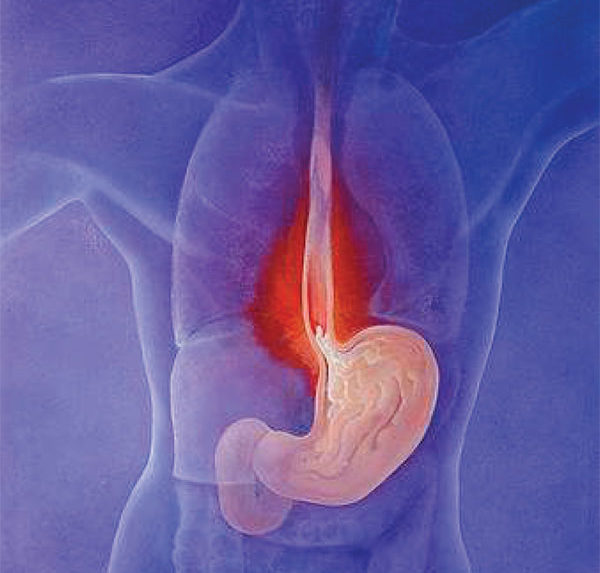
Just about everyone has an occasional bout of heartburn, or acid indigestion. That awful burning sensation around the breastbone develops when digestive juices—acids—back up in the esophagus, the tube that carries food and liquid to the stomach. When this reflux or regurgitation occurs, food or fluid can sometimes be tasted in the back of the mouth. Gastroesophageal reflux disease is diagnosed when reflux happens more than twice per week for many weeks. Between 25 percent and 35 percent of the U.S. population experiences GERD.
Not just painful, GERD can cause a variety of problems, including swallowing and sleeping difficulties, coughing, sore throat, hoarseness, chest pain, bleeding, and asthma. Over time, if the acid is not controlled, GERD can damage the lining of the esophagus leading to erosive esophagitis, Barrett’s esophagus, and, as noted, esophageal cancer.
The road to relief
Over-the-counter (OTC) antacids, such as Alka-Seltzer, or H2 blockers, such as Pepcid, which decrease acid production, can tame occasional, mild reflux. For more serious, chronic cases, the development of a class of drugs called proton pump inhibitors (PPIs) transformed treatment. Generally taken once per day, these drugs dial down the stomach’s acid pumps and help to heal the irritated lining of the esophagus.
In 2007, patients spent more than $14 billion on heartburn medications, second only to cholesterol-lowering drugs, according to IMS Health, Inc., a company that tracks prescription drug sales.
The popularity of PPIs is understandable, Katz says. “Proton pump inhibitors are such an exceptional class of drugs. They have such an excellent safety profile and are so effective at relieving symptoms due to acid that they have been widely prescribed.”
People with only occasional heartburn do not need the daily pill, but for those with GERD, “daily medication is safe,” he says. “People who take medication every day often feel better, have improved quality of life, and certainly have less symptoms” than those who take medicine intermittently.
People who require a prescription PPI, which can cost $90 to $265 per month depending on brand and dose, may soon have more and cheaper options. More PPIs are expected to become available in generic or over-the-counter forms in 2009 or soon after, joining the two generic PPIs and one OTC currently on the market. Prilosec OTC costs $19 to $26 per month and is a Consumer Reports Best Buy Drug.
“The patients do not have to worry about the expense nearly as much,” says Dr. Kenneth R. DeVault of the Mayo Clinic in Jacksonville, Florida.
Recently, the FDA approved a long-acting PPI for once-daily treatment of GERD. Kapidex (dexlansoprazole) was approved for healing all grades of erosive esophagitis for up to eight weeks, for maintaining healing of erosive esophagitis for up to six months, and for treating heartburn associated with symptomatic nonerosive GERD for four weeks, according to drugmaker Takeda Pharmaceutical.
Not Enough Relief
While PPIs are helpful to many, they are not a magic bullet.
“There’s a substantial group of patients who aren’t satisfied with the relief they get,” DeVault says. “The drugs don’t give you immediate relief. It really takes a few days to build up relief,” he says, adding that he hopes that a PPI containing sodium bicarbonate, an antacid that works quickly, will soon be sold without a prescription.
Another group of PPI users finds that the amount of acid suppression “just isn’t sufficient.” To cope, DeVault says some patients take more than the recommended one pill per day. “Probably 20 percent of people taking PPIs are taking them twice a day or more,” he estimated.
In early 2008, the American Gastroenterological Association Institute surveyed 1,064 people who used PPIs and found that nearly 40 percent still experienced GERD symptoms, such as acid reflux. Half of those surveyed used over-the-counter remedies, such as antacids, to ease breakthrough symptoms.
DeVault notes several studies have suggested that taking acid suppressants for an extended period of time could have side effects, including a higher risk of hip fractures, pneumonia, and an infection with a bacterium called C. difficile. “Those studies probably are legitimate, although the absolute risk is very, very low. If patients need acid-suppressing drugs, they should take them,” he says, adding that the patients at higher risk of side effects seem to be those taking PPIs more than once a day.
Within several years, DeVault expects to see new drugs that improve the function of the lower esophageal sphincter, the valve between the stomach and esophagus. “To me, those (drugs) are some of the more exciting things out there. They’ll probably be given to patients along with one of the acid blockers, but they’ll take care of the symptom of regurgitation, or the feeling of food coming back up.”
GERD and Asthma
Scientists are also making progress in understanding the link between GERD and asthma and other lung issues.
Physicians have observed that treating one condition sometimes leads to relief of the other. “We see patients frequently who have asthma exacerbated by reflux, and conversely, we see patients with reflux that can be exacerbated by asthma,” Katz says. “There is a relationship. It’s not clear whether it’s cause and effect.”
Reflux should be considered when a patient has difficult-to-manage, nighttime, nonallergic, or late-onset asthma. Reflux is also a consideration in patients with chronic laryngitis, hoarseness, other voice disturbances, or chronic sinus problems.
“It’s very hard to make that connection sometimes, so it requires careful thought and a careful approach,” Katz says, noting that a patient can be monitored to determine if reflux and other symptoms occur simultaneously or independently.
Chest pain is another symptom that should inspire a visit to a physician, DeVault says. Reflux and chest pain can go together, he says, but “don’t assume chest pain is indigestion.” The problem might be heart disease. A couple of times a year, he says, he sees a patient who is worried about reflux but actually has angina, which is chest pain caused by an insufficient flow of blood to the heart.
Barrett’s Esophagus and Cancer
In a small percentage of cases, GERD is a precursor to Barrett’s esophagus, a precancerous condition in which the cells lining the lower esophagus change in color, texture, and composition because of repeated exposure to acidic stomach contents. A small number of people with Barrett’s develop esophageal cancer.
Considerable debate remains over who should undergo expensive screening tests, in which an endoscope is used to view the lining of the esophagus.
“While Barrett’s tends to be most common in white men older than 50, the disease occurs in both genders, as well as all ages and races,” Katz says.
GERD and Babies
It’s normal for babies to spit up once in a while. But some infants get irritable and uncomfortable after nursing. Some scream for hours. Some refuse to eat. Instead of assuming the child has colic, some doctors are diagnosing GERD and prescribing drugs called proton pump inhibitors.
Children with GERD may have symptoms, including: repeated regurgitation, nausea, laryngitis, coughing, or wheezing. The National Digestive Diseases Information Clearinghouse suggests consulting a health care provider if your child frequently has reflux-related symptoms that cause discomfort.
Frequent reflux can cause complications, including: heartburn; esophagitis, which can develop into swallowing problems; poor growth due to poor nutrition; and respiratory problems from stomach contents entering the nose or lungs, according to the Pediatric/Adolescent Gastroesophageal Reflux Association.
Become a Saturday Evening Post member and enjoy unlimited access. Subscribe now



Comments
I have been taking Prilosec for 5 years 2 months I started having lower back aches had xrays and physical therapy that did not help then I was told that the Prilosec could be the cause so I stopped and the back ache went away in a matter of 2 days I was also told that the Prilosec could also do damage to may Kidney and or my Liver I’m searching for facts
Both my husband and myself have GERD. As the article stated, we both take prescription meds which do help the problem. A very good article.