Breast reconstruction surgeon, researcher, and author Dr. Ron Israeli, who practices in Long Island, New York, talks with Post editors about treatment options and the importance of coordinating cancer care.
When to consider
Q: A new diagnosis of breast cancer is overwhelming. At what point should women explore their reconstructive options?
A: The primary concern at the time of diagnosis is: Get rid of this cancer. Decisions are being made under fire, and issues such as breast reconstruction tend to be put aside. But a new approach, a multidisciplinary one, is being utilized at medical centers that specialize in breast reconstruction. When cancer is first diagnosed, a breast surgeon, a plastic surgeon, a medical oncologist, and a radiation oncologist provide input as to what needs to be done—and when.
Discussing options for reconstruction at the time of diagnosis may also help a woman begin to feel more comfortable about what is happening to her—she can see light at the end of the tunnel. Alternatively, she might say, “You know what, that’s not for me.” And that’s fine. She is empowered to make an educated decision about her options.
What are the options?
Q: Breast reconstruction options fall broadly into two categories: breast implants and using the patient’s own tissue. What factors determine the best approach?
A: The primary factor is the patient’s anatomy. Does she have sufficient tissue in the abdomen, back, or other areas to transplant to the chest? If so, using the patient’s own tissue is an option. When that is not the case, implant-based options are the only choice. Another factor, disease severity, may affect the timing of breast reconstruction. For example, plastic surgeons may delay using the patient’s tissue for reconstruction until radiation or chemotherapy is completed—which brings us back to why a multidisciplinary approach is so important.
How it’s done
Q: Breast reconstruction surgeons sometimes utilize a balloon-like device called a tissue expander. What is it and how does it work?
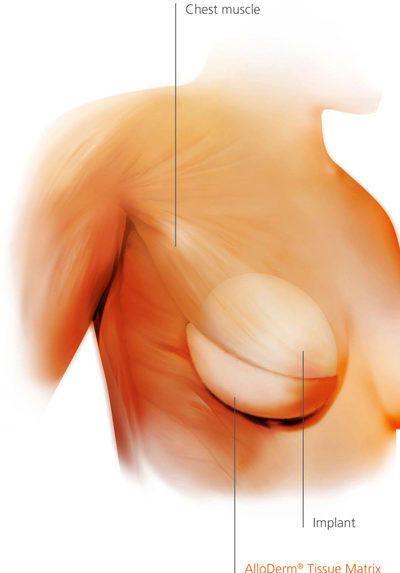
A: A tissue expander is a temporary device that is made of a material similar to plastic. We support the device with an internal sling called AlloDerm that is attached to the chest wall. After the surgery, the expander is filled with saline through a built-in port, and it slowly stretches the patient’s skin until there is enough space to perform the second stage: opening the incision, taking out the expander, and placing a final breast implant. Putting in a tissue expander mandates two stages.
What is AlloDerm?
Q: What is the sling made of, and does it remain in place?
A: We use AlloDerm, a regenerative tissue matrix derived from donated human tissue and developed by LifeCell Corporation. It acts as a replacement for tissue that is removed during the mastectomy. Through a propriety process, all of the cells are removed from the donated skin without damaging the skin matrix, preserving the biochemical components necessary for new tissue to grow into it. Basically, AlloDerm is accepted by the patient’s body and ultimately becomes a part of it.
Q: How long has AlloDerm been available?
A: AlloDerm was introduced in 1994 as a skin graft and has been utilized in thousands of burn patients without any issues. It was pioneered for post-mastectomy breast reconstruction in about 2001, and has since become the state of the art approach for breast implant reconstructions.
Q: Why is AlloDerm so helpful for breast reconstruction?
A: AlloDerm acts as a hammock for the breast implant, allowing it to lay naturally. AlloDerm also addresses some of the technical pitfalls of breast implant-based reconstruction—problems such as controlling the position of the implant, defining the fold, and camouflaging the implant. In addition, recent advances with AlloDerm allow us, in many cases, to avoid using a tissue expander and proceed directly to placing an implant. Immediately after the mastectomy, the patient wakes up with her final implant, and the AlloDerm to support it and create the breast shape. Quite frankly, we are able to achieve more reliable results than before the advent of this technique. AlloDerm provides predicable results and improved outcomes for more women than was previously possible.
Safety issues
Q: There have been concerns in the past about silicone gel implants. Are they safe?
A: New-generation gel implants have been very well studied and safety is no longer an issue. Before 1992, the gel being used in implants was so thin that if a crack developed, it would spill out and could cause local problems such as the formation of scar tissue. As a result, a moratorium was placed on the implants and, for the ensuing 14 years, a woman could get a gel implant only through a study protocol. Data was collected on thousands of women who received a new generation of implants with very viscous contents. In 2006, the FDA approved the newer implants, which have a high safety profile.
Q: What are the common reconstruction procedures that make use of the patient’s own tissue?
A: Across the country, the most common reconstruction procedure that utilizes tissue from the patient’s body is called the TRAM (Transverse Rectus Abdominus Myocutaneous flap). During this surgery, surgeons take skin and fat tissue from the abdominal area and transfer it to the chest wall. In addition, we remove and transfer the abdominal muscle that carries blood vessels needed for the skin and fat to survive. The TRAM flap procedure flattens the abdominal donor site, similar to the way that a tummy tuck works. However, removing the muscle can sometimes cause problems. In addition, it can take longer to recover from donor sites on the abdomen as compared to other areas.
Perforator flap procedures also involve transferring the patient’s skin and fat tissue from the abdomen to create a breast shape. The important difference is that no muscle tissue is removed. Instead, we tease out only the blood vessels that supply the skin and fat. Then, under a microscope, we connect the vessels from the flap to those on the chest wall in order for that tissue to survive. The most common perforator flap, the DIEP (Deep Inferior Epigastric Perforator), also allows a flat donor site. It is a complex procedure which, again, may involve a longer recovery because tissue is taken from the abdomen.
Who pays?
Q: Do most insurance companies cover the cost of breast reconstruction?
A: The Federal Women’s Health and Cancer Rights Act of 1998 protects women with breast cancer who need a mastectomy. Based on federal guidelines, the Act mandates that insurance also cover all stages of breast reconstruction after mastectomy. Women often undergo multiple stages to complete a final reconstruction. As new procedures are developed, it may take time to obtain coverage. At this point, however, all procedures that I perform in my practice—tissue expander, implant-based, and reconstructions using patient tissue, are covered.
Obstacles
Q: A recent survey from the American Society of Plastic Surgeons shows that seven of 10 women eligible for breast reconstruction don’t know their options. Why is this?
A: Old habits die hard. About 100 years ago, William Stewart Halstead, a famous general surgeon, reported the first successful mastectomy procedure for breast cancer. And he warned against reconstruction procedures because he believed that it hindered the potential for cure and might compromise the patient’s health. That belief prevailed until the early 1970s when early reconstructive procedures with implants were done. In the 1980s, general surgeons began to perform modified radical mastectomy and skin-sparing mastectomy, and new reconstruction techniques—tissue expansion and flap procedures—were developed. And breast reconstruction continues to gain popularity. Today, genetic testing for breast cancer is available. People who do not have cancer are deciding to prevent future problems by having mastectomies and reconstructions.
Yes, 30 percent is a low number, but it is definitely on the upswing. We, as plastic surgeons and the American Society of Plastic Surgeons, are aware of the reality that women living in large metropolitan areas are more likely to be offered breast reconstruction than those in small communities. But awareness is increasing and Internet information is empowering women to learn about their options. The word is getting out and the options are much more diverse than 10 years ago.
Resources
More information about breast reconstruction is available from the American Society of Plastic Surgeons, including how to find surgeons who are board certified and trained in these procedures. Click here for a comprehensive resource for breast reconstruction co-developed by Dr. Israeli and here for one sponsored by LifeCell.
Become a Saturday Evening Post member and enjoy unlimited access. Subscribe now


Comments
Thank you for a comprehensive and informative review of the options and latest advances in breast reconstruction — provided by an expert physician, who is obviously at the top of his field. As a breast cancer survivor, I can attest that the Team Approach advocated by Dr. Ron Israeli is indispensable in helping women “under fire” cope more adaptively, feel empowered and supported in their attempts to make good decisions — when their lives may be on the line with every decision, and receive the state-of-the-art care they deserve.