“Your Health Checkup” is our online column by Dr. Douglas Zipes, an internationally acclaimed cardiologist, professor, author, inventor, and authority on pacing and electrophysiology. Dr. Zipes is also a contributor to The Saturday Evening Post print magazine. Subscribe to receive thoughtful articles, new fiction, health and wellness advice, and gems from our archive.
Order Dr. Zipes’ books, Ari’s Spoon, a new novel, as well as Bear’s Promise and Damn the Naysayers, A Doctor’s Memoir. Check out his website at dougzipes.com.
Covid
Infections from delta variants of the original SARS-CoV-2 infection, particularly the subvariants BA.4/BA.5, are raging throughout the world, now causing three-fourths of all coronavirus infections in the United States. Astoundingly, half of all Covid infections since the start of the pandemic have occurred in the first seven months of 2022. While the virus strain is quite infectious, fortunately it is not as virulent as the original Covid outbreak, judged by fewer hospitalizations, intensive care admissions, and deaths.
Nevertheless, mortality is still higher than from influenza or other infectious diseases, with an annual death rate predicted to be 100,000 for at least the next several years. Patients from the most socially vulnerable communities have higher rates of mortality and major adverse cardiovascular events.
Compounding all is the risk of becoming a “long hauler,” with symptoms lasting weeks or months in 20 to 30 percent of those infected. Long haulers often suffer significant disability, including fatigue, shortness of breath, adverse cardiovascular events, cognitive issues such as brain fog, depression, and other mental health problems. People with sore throats, headaches, and hair loss soon after testing positive for COVID-19 may be more likely to become long haulers.
Ease of transmission stems from the ability of the virus to evade the neutralizing antibodies circulating in the blood in response to previous Covid infection or vaccines. The virus requires antibodies from T cells to halt its attack. Older people have more difficulty developing antibodies and more easily lose immunity over time, making Covid a disease targeting the elderly.
Also alarming is pandemic fatigue: public acceptance that this time around Covid infection is a part of everyday life rather than the threatening infection it was more than two years ago, with no or little public or governmental outcry to limit transmission. While it shouldn’t dominate our lives like in the past, it cannot be taken for granted.
The risk of reinfection is real, and people with multiple infections have a higher cumulative risk of a severe illness or death. Yet I see few people wearing masks or social distancing at indoor gatherings such as concerts, airports, stores, and restaurants.
Hopefully, booster vaccines available this fall will target BA.4 and BA.5. But if people continue to get infected, the virus can continue to mutate, and new vaccines may soon become old vaccines. We may end up fighting BA.6, 7, or 8 or a whole new Greek alphabet of viruses, some of which may be much more virulent.
So, to protect yourself and others, get vaccinated and boosted, wear masks, and maintain social distancing when appropriate. Drugs like Paxlovid can reduce severity in infected people, but rebound infections may occur after stopping.
Monkeypox
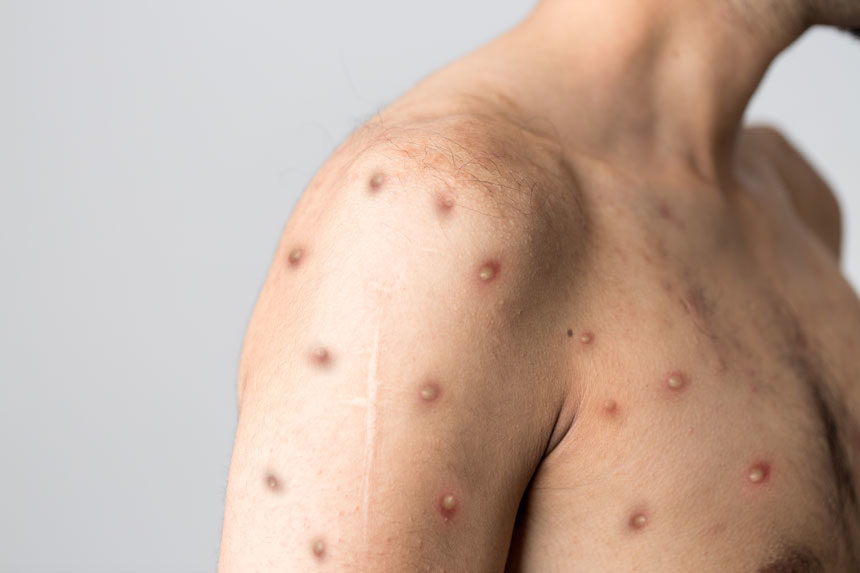
And now, adding to Covid, comes monkeypox, a poxvirus related to smallpox and cowpox. The virus was first reported in 1970 in a nine-month-old boy in the Democratic Republic of Congo, and emerged in the U.S. in 2003. Monkeypox usually causes skin eruptions in the form of pimples or blisters that typically occur on the arms and legs, but can be on mucosal, genital, and perianal areas also. Flu-like symptoms with headache, sore throat, lethargy, cough, lymph node swelling, and fever can accompany the skin eruptions.
Monkeypox is not classified as a sexually transmitted disease, though most reported infections occur in gay or bisexual men. Transmission usually occurs through close contact, including direct physical contact with lesions as well as “respiratory secretions” through face-to-face interactions. Touching objects contaminated by monkeypox lesions or fluids may also risk the spread. Monkeypox can infect anyone who comes in contact with the virus, even children. Most cases are mild and self-limiting over several weeks, and death appears to be uncommon.
At present, a limited supply of smallpox and monkeypox vaccines is available for at-risk individuals. Antiviral medications may be helpful. Vigilance is needed to contain further community spread and prevent another pandemic. WHO has declared monkeypox a global health emergency because of increasing infections. Individuals suspected of infection are considered contagious from the onset of any symptoms. They should contact a health care worker and isolate until tested and lesions heal. We should not underestimate the potential impact of this virus, and we may be just seeing the tip of the iceberg. Further information can be found at cdc.gov/poxvirus/monkeypox.
Featured image: Shutterstock
Become a Saturday Evening Post member and enjoy unlimited access. Subscribe now