Contrariwise*: Dirt is good for you
Also be sure to read 7 Microbes That are Living on You Right Now by Nicholas Gilmore.
I am not the neatest of people.
I shade more toward Oscar Madison than Felix Ungar. Don’t get me wrong: I don’t cover myself with slime, but I don’t want to live in a scrubbed-down, super-hygienic world. That’s why I’ve observed my fellow Americans’ cleanliness obsession escalate over the years with something between dismay and horror.
It’s hard even to get dirty anymore. In many public spaces, Purell dispensers seem to be replacing potted plants for decor. My pet peeve is the sanitary wipes installed at supermarket entrances, presumably so you can wipe down the handle of your cart. Really? We’re afraid of getting a few stray microbes on our hands?
This is wrong. Look at the way babies explore the world by sticking things in their mouths, says The New York Times science reporter Jane E. Brody, arguing that the practice may provide an evolutionary advantage. “Researchers are concluding that organisms like the millions of bacteria, viruses, and especially worms that enter the body along with ‘dirt’ spur the development of a healthy immune system,” she writes.
Dr. Joel V. Weinstock, the director of gastroenterology and hepatology at Tufts Medical Center, told Brody, “Children raised in an ultraclean environment are not being exposed to organisms that help them develop appropriate immune regulatory circuits.” There’s evidence that germ-free child rearing may be behind the rise in immune system disorders like MS, type 1 diabetes, inflammatory bowel disease, asthma, and allergies.
This is not to deny that public health measures of the last century, like eliminating contamination in water and food, have saved countless lives, but clearly we’ve taken a good idea and run with it to the point of absurdity.
It’s all about balance. Mary Ruebush, Ph.D., a microbiology and immunology instructor and author of Why Dirt Is Good, writes, “The typical human probably harbors some 90 trillion microbes. … The very fact that you have so many microbes of so many different kinds is what keeps you healthy most of the time.”
So, let’s stop trying to disinfect the world. It’s time to welcome a little dirt into our lives.
—Jorge Jetsohn
*“Contrariwise,” continued Tweedledee, “if it was so, it might be; and if it were so, it would be; but as it isn’t, it ain’t. That’s logic.”
This article is featured in the March/April 2017 issue of The Saturday Evening Post. Subscribe to the magazine for more art, inspiring stories, fiction, humor, and features from our archives.
Tackling Crohn’s Disease
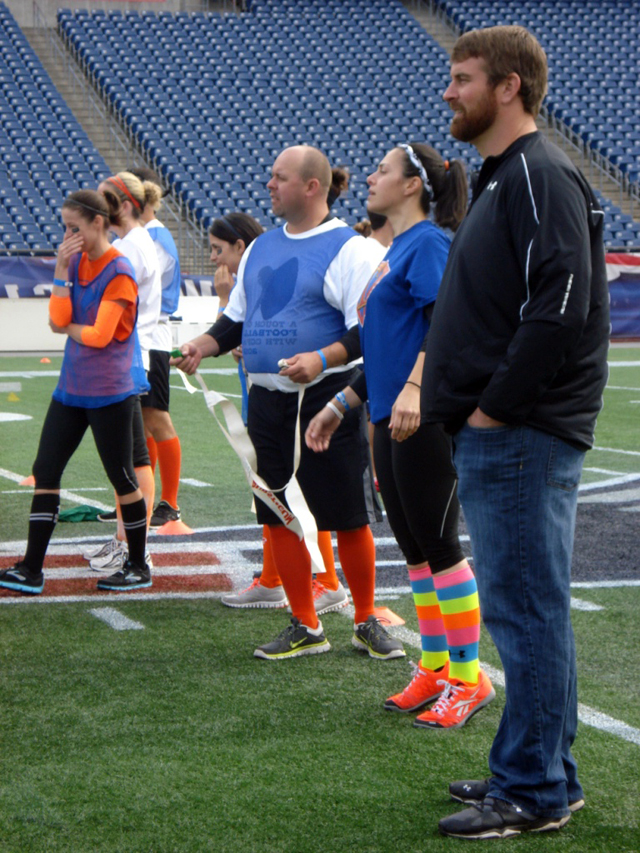
Inflammatory bowel disease, or IBD, refers to two conditions that can occur when the body’s immune system goes awry and attacks healthy organs: Crohn’s disease damages patches of the intestine along the entire digestive tract, and ulcerative colitis typically strikes only the large intestine. According to CDC estimates, 1.4 million Americans experience IBD symptoms such as abdominal pain, diarrhea, fatigue, and weight loss.
Matt Light, a record-setting tackle with the New England Patriots, was diagnosed with Crohn’s disease early in his NFL career. Now, he’s playing for a new team—the Crohn’s & Colitis Foundation of America—to raise awareness about IBD.
He credits a good mental attitude, and the prescription drug Remicade that slows inflammation, for keeping potentially life-limiting symptoms in check. “I’m proof that people can live with this really difficult condition,” he says.
Tackle Crohn’s with the ex-lineman’s game plan:
- Get educated. “Everything about testing and treatment was a surprise to me. CCFA.org is a great place to learn about living day in and day out with the disease,” says Light.
- Find the right doctor. “Having a good relationship with your doctor makes a huge difference. Look local, search out specialists, and turn to CCFA for help,” says Light.
- Connect with other patients in person or online. “It’s a tremendous help to hear the ways other people manage their symptoms and to find out what and how they eat,” he says.
Recently, the FDA approved Simponi (a drug from Janssen Biotech that’s injected just under the skin) to treat adults with moderate to severe ulcerative colitis. While the exact cause—and cure—of IBD remains unclear, researchers are testing the role of enzymes, stem cells, and bacteria in the development of these diseases. Here are some headlines worth keeping an eye on:
- Canadian Arch Biopartners Inc. say IBD is linked to a specific inflammatory enzyme called caspase 1. Hope: New tests to diagnose IBD, monitor disease activity, and gauge treatment response.
- Researchers at Wake Forest Baptist Medical Center and colleagues say a special population of adult stem cells in bone marrow can migrate to the intestine and produce intestinal cells. Hope: An injectable cell therapy to restore healthy tissue in IBD patients.
- University of California-Davis scientists say test-tube and animal studies show byproducts of IBD inflammation can fuel potentially harmful bacteria in the gut, edge out beneficial ones, and worsen the disease. Hope: Novel therapies to prevent or improve IBD symptoms.