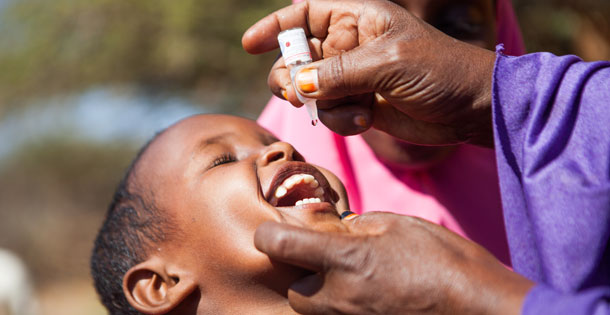
To the 4-year-old Ethiopian girl standing barefoot in the doorway of a thatched mud hut, the burly white guy beckoning to her from his wheelchair must have cut a curious figure. With eyes wide and lips slightly parted, she stepped toward him and opened her mouth as if to receive communion. And Steve Crane, 6-foot-4 and 250 pounds, held out his hand, and the blessing he gave her was in the form of a vial containing drops of oral polio vaccine.
Crane had come from Seattle to Yirgalem and Awassa, villages in southern Ethiopia, to save children’s lives, or at least to spare them from the disease that had so fundamentally altered the course of his. “I contracted polio when I was 13 years old. It was 1955, just a few months after the Salk vaccine came out,” said Crane, who added, “Ethiopia isn’t real wheelchair friendly. Rotarians had to pick me up to get over cracks in the dirt alleys, and haul me up and down stairs when we went to meetings in Addis Ababa. But it was a privilege to prevent someone else from going through what I did.” Crane was part of a group from Rotary International, whose members have been traveling, usually at their own expense, as part of the global network’s main humanitarian cause: polio eradication. Along with the World Health Organization (WHO), the U.S. Centers for Disease Control and Prevention (CDC), UNICEF, and in recent years the Bill and Melinda Gates Foundation, it makes up the Global Polio Eradication Initiative (GPEI), which has run immunization campaigns for almost 30 years.
Today, thanks to this global effort and the huge organization built to support it, the end of polio is within sight. As of November 25, 2014, there were only 306 cases. Compare that to 1988 when 350,000 people fell victim to the disease worldwide. The enormity of the achievement is hard to overstate. Some compare it to the effort to land a man on the moon. But the international infrastructure built to defeat polio — a unique collaboration in today’s fractured world — has provided the blueprint for addressing other global scourges, including malaria, measles, and, yes, Ebola too. “We now have the infrastructure,” says Oliver Rosenbauer, a spokesman for WHO in Geneva. “We have staff. We have the transportation means, the administration, the data, and the social mobilization network of local workers. That infrastructure has always been used to respond to other emergencies. Whether it’s a drought or a tsunami or the earthquakes in Pakistan, the polio teams were pulled in to help with the emergency response. The same thing is happening with Ebola. The staff in West Africa are helping, doing contact tracing, helping with surveillance, helping with social mobilization — all of that is happening in these countries and neighboring ones has well.”
Wild poliomyelitis is caused by a highly contagious virus that usually spreads through feces and enters victims through the mouth. It attacks the spinal cord and brain stem, and paralyzes arms, legs, and muscles that control breathing, swallowing, and speech. What encouraged people to think it was eradicable is that like smallpox, which was vanquished in 1979 after a 12-year campaign, people are the only reservoir in which polio can survive.
Based on Egyptian steles depicting the telltale drop foot, we know the disease has been around for at least 35 centuries. Even so, it was only in the late 18th century that polio became a full-blown global epidemic. Paradoxically, it was an unexpected consequence of vastly improved hygiene and sanitation, especially clean water and sewage removal systems in cities. When people lived in harsher conditions, they were more commonly exposed to the virus and built up immunity to it.  (Most people who get polio never know it, experiencing symptoms as mild as a touch of flu, drowsiness or a sore throat. Paralysis is quite rare, hitting one in 200 people who get the disease.) But as the world became more populated, when the virus did show up, it had a larger group to infect. In 1952, a global outbreak peaked with 600,000 cases. Photos show wards of people, unable to breathe on their own, encased in gruesome-looking iron lungs. Three years later, Jonas Salk’s injectable inactive polio vaccine (IPV) became available for public use. In 1957, another American, Albert Sabin, developed an oral polio vaccine (OPV) that contained a live, though weakened, form of the disease. And it had practical advantages: It was cheap and didn’t require any expertise to administer, so was relatively easy to deliver. Children in wealthier nations were inoculated. The last case in the U.S. was 1979 and in Britain 1985.
(Most people who get polio never know it, experiencing symptoms as mild as a touch of flu, drowsiness or a sore throat. Paralysis is quite rare, hitting one in 200 people who get the disease.) But as the world became more populated, when the virus did show up, it had a larger group to infect. In 1952, a global outbreak peaked with 600,000 cases. Photos show wards of people, unable to breathe on their own, encased in gruesome-looking iron lungs. Three years later, Jonas Salk’s injectable inactive polio vaccine (IPV) became available for public use. In 1957, another American, Albert Sabin, developed an oral polio vaccine (OPV) that contained a live, though weakened, form of the disease. And it had practical advantages: It was cheap and didn’t require any expertise to administer, so was relatively easy to deliver. Children in wealthier nations were inoculated. The last case in the U.S. was 1979 and in Britain 1985.
For years polio was fought country by country with little international coordination. In 1988 the GPEI was launched with the then-quixotic-sounding mission of stomping out the virus from the face of the earth. Thanks to the initiative, healthcare workers have since given more than 10 billion doses of vaccines to 2.5 billion children. Now, 27 years and $9 billion later, the effort is on the lip of finishing the job. In the process it has marshaled a massive coalition of governments, non-governmental agencies, philanthropic foundations, celebrities, and clerics. And it has built a meticulous infrastructure to roll the massive global program forward.
To attack polio, you need information about where the disease is, and where people are who need to be vaccinated. Stripping the concept down to its core, the process is simple: Get the vaccine from the lab to the people who need it. That’s what the GPEI has become so good at doing. When polio does appear anywhere in the world, teams are dispatched to interview families and collect samples. Then geneticists at the CDC use genome sequencing to trace the exact route the virus traveled from its source and attack it there. For example, Mideast cases that appeared in 2013 were found to originate in Pakistan; cases in the Horn of Africa came from Nigeria. Health workers in the field are equipped with GPS and detailed charts that amount to a local census, marking off every place where a child lives and has or has yet to be vaccinated. WHO estimates that as a result of the GPEI, 10 million cases have been averted and 1.5 million childhood deaths have been prevented.
For all the sophistication of the war on polio, there are battles still to be fought — some of them still being lost. In 2013, National Immunization Days had new urgency after Ethiopia, which hadn’t had a case of polio in five years, had an outbreak of nine new cases. Neighboring Somalia was the world’s worst hit with 194 children paralyzed. Kenya had another 14 cases. Nor was Africa the only flashpoint. Syria, where civil war reduced the estimated percentage of vaccinated children to 68 percent from a pre-conflict 91 percent, had an outbreak of 35 new cases. The virus also surfaced in Israeli sewage in numerous locations, prompting a mass vaccination campaign. Though no Israelis contracted polio, its mere presence raised fears of reinfection in Europe.
All this in a year when polio workers were actively targeted and murdered in Pakistan, one of the three countries left where the disease is still endemic (Afghanistan and Nigeria are the other two). Although no one claimed responsibility, suspicion fell on radical Islamists. To be clear, support for eradication has been mostly robust throughout the Muslim world. Saudi Arabia requires proof of vaccination for all pilgrims from polio stricken areas as a condition of making hajj, the journey to Mecca. The Islamic Development Bank has made financing available to Pakistan. Malaysia, Qatar, and Kuwait have helped with financing and technical assistance, while Abu Dhabi hosted a major summit in 2013. But extremists remain a source of consternation to the polio community. “I don’t think there’s any question that polio eradication is impacted by anti-government groups in places like Afghanistan, Pakistan, Somalia, and Nigeria,” says Carol Pandak, director of Rotary’s PolioPlus program. “They’ve made it difficult to access children.”
The Ebola outbreak, too, threatens to hinder polio eradication efforts, particularly in Africa where the risk of Ebola threatens to impede the movement of polio workers. In fact, the timing of the Ebola outbreak could hardly be more frustrating: With just six polio cases in 2014 as of this writing, Nigeria is closer than ever to eradication. Ebola could prove to be a major setback. “We might only have a limited window of opportunity to finish polio,” says WHO’s Rosenbauer, “If Ebola got into northern Nigeria it would complicate polio activities.” Despite setbacks, there have been triumphs. In January 2014, India, once considered the disease’s most intractable redoubt, marked 36 months without a new case, allowing WHO to certify the Southeast Asia region polio-free. Of the countries where polio still persists, as of November 25 Nigeria had only a half-dozen new cases in 2014 compared with 50 for roughly the same time period in 2013; Afghanistan had 21 cases, compared with nine in 2013; and Pakistan, where warlords in Waziristan cut off access to vaccine, was the real dark spot with 260 cases, compared with 64 in 2013.
The fear of failure is ever-present for the GPEI. “Until it’s completely eradicated, it can flare up again,” says Dr. John Sever, a pediatric infectious disease specialist and vice chairman of Rotary’s International PolioPlus Committee. “If this spreads into populations that are not well-immunized, it could cross borders and re-infect areas that are currently polio-free.” The worst setback — remembered as “the disaster” — occurred in 2003 after rumors spread that vaccination was a Western plot to sterilize Muslim children. That shut down the Nigeria campaign for 13 months and led to reinfection in 20 countries. More recent rumors had it that vaccinators were fronting for Western intelligence agencies — and it hardly helped that the doctor who led U.S. troops to Bin Laden had in fact set up a fake vaccination clinic.
As massive as the cost of eradication is, the price of failure is higher. An economic analysis in the journal Vaccine in 2010 determined that without total eradication, the disease would run up a bill as high as $50 billion by 2035 — a figure that dwarfs the projected 5-year budget of $5.5 billion the GPEI says it needs to complete the mission, including a post-eradication plan that runs through 2018. The money is not fully available:  “We have approximately $4.9 billion in funds and pledges against the $5.5 billion we need,” says Rotary’s Pandak. “Only $1.8 billion of the pledges have been operationalized. The challenge is to realize those commitments as soon as possible.”
“We have approximately $4.9 billion in funds and pledges against the $5.5 billion we need,” says Rotary’s Pandak. “Only $1.8 billion of the pledges have been operationalized. The challenge is to realize those commitments as soon as possible.”
The legacy of eradication, advocates say, is an infrastructure of people and systems that other health programs will inherit — and that brings us back to the Ebola crisis. The two diseases are radically different and require different interventions. But Ebola reinforces exactly why the weak links in the chain of global healthcare need to be strengthened, and the network and methods of the GPEI — personnel, disease surveillance, communications structure, social mobilization, emergency preparedness plans, and logistics including the physical delivery of medicine and supplies — may be the best model.
Polio helped build up the capacity of countries with poor health systems, including a global laboratory and a communications network. There are now tens of thousands of health workers trained in containment of infectious disease. As a result, not just Ebola, but measles, malaria, and dengue fever are in epidemiologists’ sights. The polio endeavor fostered a better understanding of how to move science from the lab to the people in the streets and villages.
Most people who have participated in the polio effort can recall a moment when they became wedded to the mission. Ann Lee Hussey got polio in 1955 and suffers post-polio syndrome, the severe and lasting after-effects that can strike decades later and be intensely painful and disabling. Despite that, Hussey has been on 25 campaigns in seven countries including Mali, Bangladesh, and Nigeria. “It’s very healing to give the drops,” says Hussey. “It’s where I get my strength from. When I think of the faces and the people I met, I want to go again. It’s what keeps me going.”
Become a Saturday Evening Post member and enjoy unlimited access. Subscribe now



Comments
Great article