We are pleased to bring you Your Weekly Checkup, a regular online column by Dr. Douglas Zipes, an internationally acclaimed cardiologist, professor, author, inventor, and authority on pacing and electrophysiology. Dr. Zipes is also a contributor to The Saturday Evening Post print magazine. Subscribe to receive thoughtful articles, new fiction, health and wellness advice, and gems from our archive.
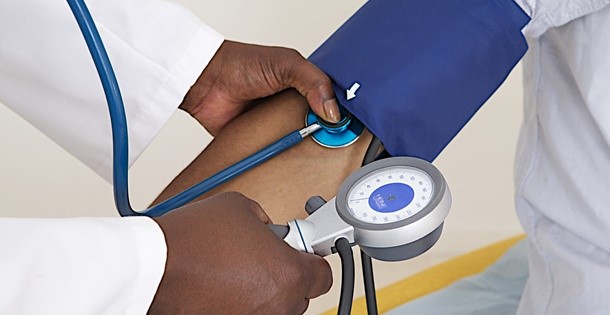
My blood pressure (BP) has kept pace with my age, slowly creeping up despite a healthy life style. Aging blood vessels become less pliant and cause BP to rise in older people. Psychosocial stress can also play a role. Recent estimates indicate that almost 900 million adults worldwide have a systolic BP of 140 mm Hg or higher, with 80% of people older than 75 years being hypertensive.
It s not by accident that hypertension, one of the leading causes of heart disease and stroke, is called the silent killer. In its early stages, an elevated BP produces no symptoms even as the constant pounding begins to take its toll on kidneys, heart, brain and other organs. Symptoms appear when these organs show the effects of wear and tear: kidney failure, heart attacks, heart failure, and strokes. Fortunately, my astute physician spotted the BP rise early and instituted appropriate treatment. Older patients benefit most from controlled BP, experiencing reduced cardiovascular and kidney disease, strokes, and mortality.
What is a normal blood pressure? Experts have recently reevaluated hypertensive guidelines, defining the various BP stages as follows:
- Normal: Less than 120 systolic/80 diastolic mm Hg
- Elevated: Systolic 120-129 and diastolic less than 80 mm Hg
- Stage 1 hypertension: Systolic 130-139 or diastolic 80-89 mm Hg
- Stage 2 hypertension: Systolic at least 140 or diastolic at least 90 mm Hg
- Hypertensive crisis: Systolic over 180 and/or diastolic over 120 mm Hg, with patients needing prompt changes in medication if there are no other indications of problems, or immediate hospitalization if there are signs of organ damage.
Who should be treated and with what? Initially, lifestyle modifications including the DASH diet (Dietary Approaches to Stop Hypertension: reducing salt and processed foods; eating potassium-rich fruits and vegetables, whole grains, low-fat dairy foods, and lean sources of protein), exercise, weight loss, moderate alcohol consumption, and stopping smoking should be adopted by everyone.
Medications are recommended for Stage I hypertension if a patient has already had a cardiovascular event such as a heart attack or stroke, or is at high risk of heart attack or stroke based on age, the presence of diabetes mellitus, chronic kidney disease or calculation of atherosclerotic risk.
The biggest risks of intensive BP therapy are dizziness on standing in frail elderly patients and acute kidney injury in patients with long-standing diabetes and kidney disease. Because coronary heart disease (atherosclerosis) goes hand-in-hand with hypertension, statin therapy is indicated for many patients with hypertension. Medication non-adherence is a major cause of apparent drug-resistant hypertension and adverse cardiovascular outcomes.
There are lots of things in life beyond our control that can influence our health: genes, sex, and age, for example. However, regulating BP is one risk factor we can control to reduce many adverse outcomes, particularly as we grow older. Check with your doctor. Monitor your BP. You ll be glad you did.
Become a Saturday Evening Post member and enjoy unlimited access. Subscribe now