Donna was in her mid-60s, with wide brown eyes and the smoky voice of a jazz singer. Her skin, sprinkled with freckles and sunspots, stretched tightly against her delicate cheekbones and jaw. It was an unusually balmy afternoon in San Francisco, and somehow the day’s heat and humidity had made its way into her room on the 14th floor of the usually chilly university hospital. Donna grasped a handheld electronic fan, closing her eyes as it cooled her face and tousled strands of the thin gray-brown hair that brushed her shoulders. When I met her, I was a fourth-year medical student weeks away from graduation, yet increasingly uncertain that medicine was the right career for me.
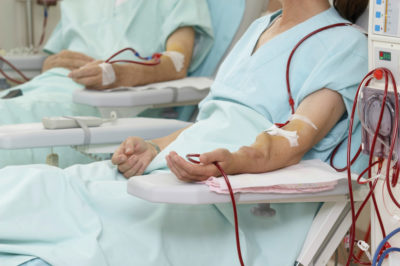
Five years earlier, Donna’s kidneys began to fail from a combination of high blood pressure and diabetes. She was weak and nauseated, and missed so many days at work that she nearly lost her job as a secretary in a contractor’s office. In order to feel better and to survive, Donna had to begin dialysis, a three-hour-long treatment three times a week that would clear her blood of the waste products and toxins that her failing kidneys could no longer remove. A vascular surgeon operated on Donna’s arm to create a fistula, a connection between an artery and vein that enabled the dialysis machine to remove, clean, and return all of Donna’s blood to her body. For the first few years, dialysis not only staved off death but actually improved her energy and outlook. She went back to work part-time. Her nausea vanished, and she managed to gain back the 10 pounds she’d lost when kidney failure claimed her appetite.
Medical school had been far more technical than humanistic, its emphasis heavy on the science of medicine, light on the art of doctoring.
But a few years later, her nausea and fatigue returned; dialysis began to cause the symptoms it had once fixed. Donna cycled in and out of the hospital with severe infections of the skin around her fistula and blood clots that plugged her fistula, rendering dialysis impossible. During a recent hospitalization, a team of physicians had placed a temporary dialysis catheter in one of the large veins in her neck while another team worked on repairing her fistula, which had clotted again. Yet she returned to the hospital several weeks later with a severe pneumonia, likely caused by powerful bacteria she’d been exposed to during her last hospital stay. When she finally left the hospital, she needed three weeks’ worth of physical therapy in a nursing home before she was strong enough to care for herself at home. Though she was able to return home, she struggled to dress herself, cook, or drive to her dialysis sessions every Monday, Wednesday, and Friday.
She had come to the hospital today because a blood clot once again clogged her fistula. Her doctors wanted to place another temporary dialysis catheter and consult a vascular surgeon to create a new dialysis fistula altogether. But Donna said no.
I don’t want dialysis anymore, Donna told her doctors. I’ve lived a good life.
If Donna doesn’t want dialysis, her doctors wondered, then what does she want and how should we treat her? These were questions I had rarely encountered or considered in my years as a medical student. Like the doctors who taught and supervised me, I was hardwired to preserve and prolong life. On the few occasions I’d seen patients opt out of lifesaving treatments, I’d watched my supervising doctors struggle to articulate another plan — and the consequences and limits of any plan at all. Donna’s team knew they needed help having that sort of delicate conversation with her, so they called the palliative care team to speak with Donna and help clarify what she wanted if she didn’t want dialysis.
As it happened, I met Donna because I had chosen to spend two weeks of elective time on the palliative care service at the University of California, San Francisco, where I was finishing my last months of medical school before beginning three years of residency training in internal medicine. I’d completed all of the required rotations to graduate, having spent one to two months each learning from teams of internal medicine physicians, gynecologists, family physicians, surgeons, pediatricians, psychiatrists, and neurologists. Now, in these last months of medical school, I’d been able to choose which medical specialties I wanted to learn, and which doctors I wanted to learn from.
I searched the list of electives for inspiration. Medical school had been far more technical than humanistic, its emphasis heavy on the science of medicine, light on the art of doctoring. In the first few years of medical school, I understood why this might be the case: I couldn’t diagnose and treat patients without an expert understanding of the body’s physiology, the ways disease could alter it, and the proper ways to treat the dizzying myriad illnesses humans suffered. Yet during my rotations, when I actually saw patients under the guidance of a resident and attending physician, I’d been struck by how little time I spent with patients — no more than a few minutes on rounds, and occasionally a few more minutes later in the day, when absolutely necessary. Caring for patients somehow meant spending very little time with them. One day, out of curiosity, I timed myself completing my assigned tasks. I spent twice as long in front of a computer as I did examining and talking to my patients.
As graduation and the start of residency loomed, thoughts of quitting medicine arose unbidden in my mind. When I looked through the list of electives I could take, I was really searching desperately for reasons to finish my training. I’d go on to spend a month working with a psychiatrist who specialized in treating patients struggling with substance abuse. I’d spend another month working with a child abuse response team at the county hospital. A classmate recommended that I take a two-week-long rotation with the palliative care team, and I found myself signing up for an elective with them, too.
One day, out of curiosity, I timed myself completing my assigned tasks. I spent twice as long in front of a computer as I did examining and talking to my patients.
Donna was the first patient I’d see with Dr. McCormick, the physician on the palliative care team during my rotation. A handsome man with gentle brown eyes and a warm smile, Dr. McCormick wore a blue plaid shirt and khakis and worked closely with a social worker and a chaplain named Ellen. We sat together around a rectangular table and talked about each of the 12 patients our team was seeing, including Donna, our newest referral. “Sounds like the medical team wants to do what they can to help Donna continue dialysis, but she’s not digging that plan,” Dr. McCormick said, summarizing the dilemma that Donna’s doctors needed us to address. “So let’s go find out what she’s got on her mind!” He was casual and personable, professional but not distant. As we walked together down a set of hallways to Donna’s room, it struck me that Dr. McCormick had never met Donna before. I wondered how he, a stranger at the eleventh hour of Donna’s life, would manage to earn her trust and ask her intimate questions that it seemed nobody had asked her before, including the many doctors who had been taking care of her since her kidneys began to fail.
Instead of hovering over her or leaning against the wall as she spoke, Dr. McCormick, Ellen, and I sat in gray folding chairs facing Donna. Dr. McCormick spoke to her in a soft tone that exuded compassion and presence. “We are from the palliative care team, and we’re just here to get to know you and to support you as you think through some of the decisions your medical team is asking you to make,” Dr. McCormick said.
“I need … all the support … I can get,” Donna replied, her voice fading into a whisper as she made her way through her sentences.
Dread had consumed Donna on the ambulance ride from her dialysis center to the hospital. She told us she had felt her heart thumping against her chest as though it were warning her of impending danger. She knew her doctors would offer her another procedure or surgery to fix her fistula and allow her to continue dialysis. But a question surfaced in her mind, one she’d considered from time to time over the past several months: Would a shorter life without dialysis be better than a longer life with dialysis?
“I’m not suicidal,” she whispered. “I’m tired.”
She told us about the many ways that dialysis had enabled her to enjoy the past five years. She would miss her adopted daughter and the view of the Bay Bridge from her front porch. She would miss making her mother’s recipes for barbecued ribs and lemon tart. But she wouldn’t miss the crushing fatigue of kidney failure that had slowly deprived her of one independence after another: The ability to use the toilet in her Spanish-tiled bathroom. The pleasure of taking a shower alone, scrubbing herself with lavender body wash, standing rather than sitting in a plastic shower chair. The full sensory immersion in her garden, hands deep in the fragrant earth as she tended her marigolds and daisies, leaving behind imprints of her knees in the soft dirt.
“I am sorry this has been so tough for you,” Dr. McCormick said to Donna, handing her a box of tissues. “I hear you saying that dialysis has really helped you to live well and to enjoy your life, but I also hear that over the past year it’s really been making you tired and sometimes it’s even made you sick.”
“Yes, it has,” Donna said, pausing to catch her breath. Even crying wore her out.
“Have your other doctors talked with you about what stopping dialysis would mean?”
I held my breath, unsure exactly what Dr. McCormick was asking. Did he want Donna to say out loud that she knew she would die without dialysis?
“Honestly … they didn’t really … say too much,” she said, wrapping thin shreds of tissue paper around her right index finger. “What would … happen to me?”
“Well, the first thing you need to know is that it is okay for you to want to stop dialysis if it is not helping you to live well,” Dr. McCormick began. “But it is also very important for you to understand what would happen without dialysis. The toxins that dialysis usually removes from your blood would build up.”
“And then … I would … die?” Donna whispered.
“Yes, you would die from your kidneys failing,” Dr. McCormick replied. I had never seen a doctor tell a patient so directly that they would soon die. I’d seen well-intentioned doctors try to soften the blow of hard facts by cluttering their sentences with rambling apologies or canned reassurances, talking around the truth. Their worry that a patient might be unable to handle plainly stated facts, that they must require unnecessary words and sentiments as a sort of shock absorber, struck me as a form of paternalism. Dr. McCormick’s sentences, concise and compassionate, almost felt transgressive. I had never seen a doctor disclose a wrenching truth with acceptance rather than avoidance. His voice was steady and clear of euphemisms like “passing on” or “being at peace.” I waited for Donna to stop the conversation, to say that discussing death so openly overwhelmed her. But all she did was nod. It was as though Dr. McCormick had validated what she already knew, as if she found this statement of truth comforting. “But our focus would be making sure that you are comfortable and free of any suffering during that time.” He looked Donna in the eyes, placing his hand respectfully on her shoulder and nodding his head deeply to emphasize the last part of his sentence.
“How would … I suffer?” Donna asked, suddenly looking at me. Even though after years of studying I could tell Donna everything about how her kidneys work and what happens to her body when they fail, I hadn’t the slightest idea how she would experience dying from kidney failure, or what medications could ease her suffering. My silence stunned me. I struggled to understand how I could be on the cusp of becoming a physician and lack the words to answer her question, to guide her through the one certain transition every patient of mine, every human being including myself, would experience.
“When you stop dialysis, one of the most common things that happens is that the fluid that dialysis usually takes out of the body can build up in the lungs, and you can have some difficulty breathing,” Dr. McCormick began, and Donna nodded. “So I would give you medicines to help prevent any gasping or difficulty breathing you might have.”
“Good,” Donna whispered, adding, “I don’t … want … to suffocate.”
“There are two medicines I will make sure we give you so that you don’t experience that awful feeling,” Dr. McCormick said. “The other thing that can happen is that the toxins that build up when you stop dialysis can make you confused and eventually sleepy. Usually this isn’t painful, but it can worry those around you.”
(Shutterstock)
“I don’t … want pain,” Donna responded, and Dr. McCormick quickly reassured her that kidney failure generally doesn’t cause pain, and death would arrive only after loss of consciousness. Kidney failure, he told her gently, could be a very merciful way to die.
I had never seen this type of doctoring before.
As the conversation unfolded, I felt a knot in my stomach harden, realizing the enormous implications of Donna’s statements. Intellectually, I knew that patients could choose not to start a treatment or discontinue a treatment that wasn’t helping them, but I had never witnessed a patient say that their quality of life was actually worsened by a treatment intended to help them live.
“I’m ready,” Donna whispered. “I know … God is … waiting for me,” she whispered. Chaplain Ellen took Donna’s hand and asked her if she found solace in religion or spirituality. Donna nodded, whispering that she was a Christian, asking Ellen to pray with her. As Ellen read from the book of Psalms, Donna’s shallow breathing slowed, her face relaxing. “When the righteous cry for help,” Ellen read, “the Lord hears and delivers them out of all their troubles. The Lord is near to the brokenhearted and saves the crushed in spirit.”
“Thank you, sister,” Donna whispered.
The dying I had encountered prior to meeting Donna had been either sudden and unexpected (the result of a terrible car accident) or a failure of the most aggressive possible medical treatment (the man with advanced cancer who died after 25 minutes’ worth of CPR). In retrospect, I realize that these were examples of death. Dying was a process I hadn’t been able to recognize during my years of medical school. I felt tears burn at the corners of my eyes and blinked them away, willing myself to stay composed. But I wasn’t sad for Donna. I admired her.
Here, at the very end of medical school, mere weeks before I became a “real” doctor, I finally saw what it meant to care for a dying patient. What emerged as I listened to Dr. McCormick’s conversation with Donna was different from taking a social history, a brisk collection of essential facts about a patient’s life that could impact their health. I had always taken pride in memorizing facts about my patients that helped me to understand who they were: their children’s names, their birthplaces, and their jobs. But those were still just facts, ones I collected earnestly because this felt like the closest I’d ever come to knowing my patients as people, seeing them as human beings, despite the ways in which medical training placed an increasing distance between us. This conversation with Donna was different. It was about understanding what truly mattered to her, and how she could make choices about her medical care that would privilege rather than sacrifice her priorities.
Up until this point, I’d come to believe that treating disease was the best way to alleviate suffering. The person and her disease collapsed together, the boundaries between the two ever more indistinct as medical school continued. But by unintentionally treating patients like a panoply of diagnoses, biological mysteries to be solved, I was losing sight of what had drawn me to medicine in the first place: the unique opportunity to become both a scientist and a humanist, translating book knowledge into relief of human suffering. The cumulative challenge of memorizing endless maladies and their treatments, rushing around the hospital to see patients and order lab tests and call consultants, the pressure to perform well, and the long hours in the hospital wore on me, even as the meaning I found in the work waned. During my palliative care elective, though, that meaning began to return. How ironic, I thought, that I began to find my purpose in a field that embraced what medicine sought to erase.
Over the next two weeks, Dr. McCormick taught me how to properly evaluate and treat pain and nausea, basic symptoms I realized I didn’t feel prepared to treat even though I was on the verge of completing medical school. Dr. McCormick taught me the difference between hospice and palliative care: hospice isn’t a place, but rather a type of palliative care that teams of nurses, doctors, social workers, and chaplains provided to patients, often in their own homes, when they had less than six months to live. I took notes as I watched him lead family meetings, asking patients about how the realities of their diseases reshaped their hopes and goals.
I hadn’t considered that patients could have goals other than fixing a medical problem and returning home. I listened as a patient dying of pancreatic cancer told Dr. McCormick that she wanted to feel well enough to attend her daughter’s college graduation in two months. An elderly gentleman found the courage to tell us that appointments with his oncologist took up too many hours of his waning life; he’d rather be at home with the family he loved than driving back and forth to the oncology clinic, spending hours in a cushioned chair as chemotherapy dripped into his veins. Though many of the patients I cared for were dying, we spoke mostly of their lives, of what it meant to live well in the time they had remaining.
Although she had hoped to die at home with the support of hospice, Donna became confused and then slipped into unconsciousness three days after we met her. We stopped by her room several times a day, carefully adjusting doses of her medications to ease her shortness of breath, confusion, and pain. Her family tied balloons to her bedpost and surrounded her with photographs of people who loved her. They encircled her and sang, the melodies of hymns fractured by their tears. She died in the middle of the night shortly after her family left, alone in a quiet but peaceful room.
What I learned from Dr. McCormick and Ellen was so distinct from what I’d learned and experienced in medical school that I wondered if it was “real” medicine. The medicine I’d learned was fast-paced and lifesaving, an enterprise that relied on plastic catheters and ultrasounds, operating rooms and endoscopy suites, a rainbow of pills for diabetes and high blood pressure, saline and antibiotics that coursed through the body from bags attached to an I.V. pole. The effort to extend life left no space for accepting death.
When I look back on those two weeks, I realize that I did not do for my patients what I had been trained for years to do: I did not diagnose or fix their ailments. They didn’t live for more than days or weeks after I met them. But it is not their deaths that I remember. It is the peace they found in the honesty we offered, in the opportunity for them to articulate their suffering and what they wished for in the time they had left. During those weeks, I’d felt both human and humane, like a person and a doctor rather than one or the other. I left my rotation feeling the closest I had felt to the doctor I always wanted to be.
From That Good Night by Sunita Puri, published by Viking, an imprint of Penguin Publishing Group, a division of Penguin Random House LLC. Copyright © 2019 by Sunita Puri.
Sunita Puri, M.D., is the medical director of the Palliative Medicine and Supportive Care Service at the Keck Hospital and Norris Cancer Center of the University of Southern California. She has published essays in The New York Times, Slate, and the Journal of the American Medical Association.
This article is featured in the July/August 2020 issue of The Saturday Evening Post. Subscribe to the magazine for more art, inspiring stories, fiction, humor, and features from our archives.
Featured image: Shutterstock
Become a Saturday Evening Post member and enjoy unlimited access. Subscribe now



Comments
I wish my husband could have read this and experienced the palliative care modeled here before his death. Over a period of about 45 years he experienced major medical problems and several times was given a 50-50 chance. He always fought through and outlived the treatments he received in many cases. In 2012 he had to go on dialysis, began experiencing difficulty swallowing, and had problems due to complications of a 1991 major surgery; had aspiration pneumonias, bladder cancer, diabetes, etc., etc., etc. Suffered from frequent GI bleeds, and was anemic and kept losing weight and strength. His last year of life was extremely painful, difficult, and caused him to be unable to do much or even enjoy visits from family and friends who had been important to him all his life. He frequently reiterated that he was ready to go and didn’t understand why God didn’t take him home and that he was tired. He suffered physically and emotionally.
This article should be required reading for every medical student before graduating from medical school. It astounds me how many doctors have no clue about what is important to the patient. I am in my 80’s and so far I have found only ONE.
In 1985, when I became a “hands-on” patient care volunteer for hospice (no hospital affiliation at that time), I learned valuable lessons about families and dying patients and thought to myself that every doctor and nurse and medical personnel should be required to take the hospice training classes that I had just completed. I am happy to see that palliative and hospice care has, albeit not fully, been incorporated into patient care. What a tremendous blessing for families and the dying patient to have understanding and a caring connection to their medical team.
Death is part of life; it is true the “efforts to extend life by whatever means has gone too far in many instances.”
Thank you for this article, Dr. Puri. You learned one of the most important aspects of being a doctor after completing medical school but before becoming one officially. I, along with you, feel you were very lucky to have gotten to work with Dr. McCormick in regards to Donna, and what SHE wanted, easing things for her with honesty and empathy as she transitioned into the other side of life.
The efforts to extend life by whatever means necessary has gone too far in many instances. It is something on a case by case basis, and I think doctors in general have been ‘hard wired’ away from discussing death in situations like Donna’s. It’s really not their fault for this very reason. You were blessed to work with a such a doctor and Chaplain Ellen. I can feel the reassurance they gave her, along with yourself.
I can’t even imagine what the C-19 situation has done to our doctors, nurses and all front line workers psychologically, mentally and physically, far beyond overwhelmed with the relentless horror and terror with the massive numbers of patients being brought in round the clock 24/7 all these months. So much of it could be halted if large social gatherings would stop, everyone wore the mask, and we weren’t getting (once again yesterday) insane medical ‘advice’ from the President. We don’t have a vaccine for this yet, but there is plenty we CAN do to offset it in the meantime.